In most cases pressure ulcer prevention can be accomplished by risk assessment followed by common sense choices for pressure reduction. In these days of evidence based medicine, health care providers need to listen to the evidence and implement best practices to reduce the incidence and prevalence of adverse outcomes such as pressure ulcers.
 An important research article on pressure ulcer prevention recently came out in the Journal of the American Geriatrics Society. This article proved what wound care clinicians already know – that special seating cushions in conjunction with properly fitted wheelchairs prevent pressure ulcers.
An important research article on pressure ulcer prevention recently came out in the Journal of the American Geriatrics Society. This article proved what wound care clinicians already know – that special seating cushions in conjunction with properly fitted wheelchairs prevent pressure ulcers.
Improper wheelchair seating is an identified risk factor for pressure sore development. Many wheelchair users suffer from seating discomfort and high sitting interface pressures. Wheelchair cushions provide part of the solution, but must be accompanied by proper wheelchair fit to accommodate basic principles of body mechanics.
Researchers assigned nursing home residents into two groups. The control group was not given a wheelchair and seating assessment and received a segmented foam cushion (SFC) not specifically designed for pressure redistribution. The experimental group received a wheelchair mobility and seating assessment and a skin protection cushion (SPC) selected through pressure mapping. It is no surprise that the experimental group had a statistically significant finding of fewer pressure ulcers.
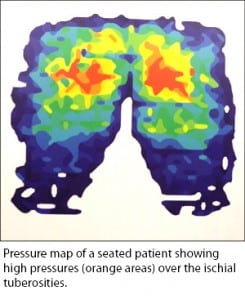
Seating acquired pressure ulcers were defined as occurring in the ischial tuberosity area Sacral ulcers were excluded as they occur primarily when supine in bed. Average age of residents was in the mid-80’s and the group had multiple comorbidities and severe mobility limitations.
Pressure mapping was used to assist selection of proper wheelchair cushions. Pressure mapping uses a computer based sensor pad that gives digital readings of pressure information, showing areas of high and low pressure when seated. The authors acknowledge that although pressure mapping is considered a “best practice” it is generally not used for most nursing home patients.
The authors conclude that residents who are wheelchair bound and at risk for pressure ulcers should be provided with a wheelchair mobility and seating assessment, properly fitted wheelchair, and skin protection cushion. Given the enormous cost of pressure ulcers as well as the associated morbidity, investment in preventive technologies such as pressure mapping for choice of seating options may not be a bad idea.
* * * * * * * * * * * * * * * *
Similar posts:
Pressure Ulcer Prevention Lacking in High Risk Patients
Optimizing a Hospital System to Prevent Pressure Ulcers
New Research Sheds Light on Hospital Acquired Pressure Ulcers
The reference for this post was: Brienza et al. A Randomized Clinical Trial on Preventing Pressure Ulcers with Wheelchair Seat Cushions. J Am Geriatr Soc. 2010 Dec;58(12):2308-14.

Pressure mapping has to be done by knowledgeable and skilled clinicians. You can’t just buy a fancy machine and start plopping people down on it.
Just like statistics, pressure mapping can be used to show whatever you WANT it to show. You can change the settings to make it more or less sensitive, you can use people of different weights and shapes, you can position them in various ways to make the map look however you want it to look.
Most clinicians have no clue how to read a pressure map, they just look at the colors to see where the red is. They don’t consider if the red is over a flat bone or a pointed one, they don’t consider redistribution of pressure, only if all the colors look relatively the same. They don’t consider what pressures a particular color means on this particular map, or what the height and weight and body mass distribution is of the subject, or even which mapping device was used.
In unskilled hands, and read by unskilled eyes, mapping is useless, but can be a great marketing tool.
Thank you so much for your comment Laurie. My own experience with pressure mapping has been limited, but I know that some wound clinicians rave about it. Perhaps your observations reveal why pressure mapping is still not considered the standard of care.
I would like to echo Lauri Rappi’s comments. Pressure mapping has been used by one major wheelchair cushion manufacturer as the “end all, tells all” of pressure sore prevention and the proof that it is not is in the high incidence of sores acquired by people using these cushions. That manufacturer has pretty much written the book on how pressure mapping is done and interpreted. Most physical therapists get their pressure map reading training by way of this manufacturer and simply don’t know any better.
Pressure sores are not caused by pressure alone but are caused by pressure combined with lack of movement! When movement is recreated by artificial means people who have a long and dismal history of recurrent pressure sores find they can stay up in their chairs as long as they want without pressure sores. My patented alternating pressure custom built wheelchair cushions are doing exactly that for hundreds of people every day and yet the medical community still relies on static non- moving cushions. I have had hundreds of customers in the last 10 years who have previously had flaps, grafts and cumulatively months of hospital confinement get on our system and have not had any more pressure sores.
Four years ago the US Air Force discovered they had a real problem when the B-2 bombers were bombing Iraq. Some of these pilots sat in an ejection seat for as long as 48 hours with a 1″ pad of memory foam over a molded fiberglass seat, belted down so securely that movement was very restricted. Many of them suffered pressure sores and so did many of the air crews in other long duration flights. The Air Force did something that has NEVER been done in the medical community to my knowledge. They bought examples of virtually every cushioning concept that was advertised to “prevent” pressure sores. They set up a scientific study at Wright Patterson AFB in Ohio and tested every aspect on human subjects sitting for long periods in simulated cockpits. No manufacturer had any inkling that this was taking place so the testing was completely unbiased and positively results based.
They had purchased 2 of our commercial cushions and tested them even though they have never been sold as “medical” cushions. Based on almost 2 years testing we were contacted and contracted to build 2 prototype cushions specifically designed for an ejection seat to military standards. We did this and then gained 2 contracts for cushions to be tested in various military aircraft. Now, the B-2 bombers are equipped with our alternating pressure seat cushions and we have licensed our patent to Goodrich Aerospace for military aircraft only. We have hundreds of customers living amd more importantly working pressure sore free, some for as long as 10 years now, and can back up everything I have said here with facts.
Why is the medical community still messing around with static cushions when infinitely better cushions are available? I think the answer is money, Medicare will not pay more than $500.00 for a cushion and will not do anything to prevent pressure sores, they seem to prefer paying for hospitalizations. Among my customers, I have lawyers, preachers, school teachers, a machine shop owner, several independent business men and all of them are working and paying taxes rather than suffering recurrent pressure sores, paid for by public money.
Dr., this reply is to you rather than a bid to have my say on your website. If you have an open mind, I can and will prove to you that at least 85% of sitting related pressure sores can be totally prevented with existing technology. Our government spends from 7 to 11 BILLION dollars a year treating pressure sores and I firmly believe that fully 80% perhaps even more could be prevented. Better yet, many of those same people could be living happier, healthier and productive lives, earning their own living instead of being treated for pressure sores. I hope you will be interested enough to contact me. I’m not a medical person but am a pretty good engineer who has a better way to control the incidence of pressure sores and thats a fact easily proven.
Thank you in advance for any response. Rex Taylor, CEO at Ease Seating Systems. Please do look at my websites: easecushion.com, and thebestseatever.com.
The reason that I have sent you this note is that your response to Laurie Rappi’s letter seems to indicate an open mind and willingness to consider other views.
Thank you Rex for this thought provoking comment. I have used alternating pressure air mattresses (APAMs) in nursing homes for bed-bound patients but have never seen this technology applied to seating. It really sounds like a great idea.
A good wheelchair seat cushion for your chair is too important to be considered a luxury item and you should find one that fits your requirements exactly. A good cushion can save you not only from pressure sores but also from the incorrect posture that can generate a variety of back and neck problems. If you have a neuromuscular disease, respiration, circulation and swallowing are also concerns that need to be addressed by correct posture, which means being supported by a good cushion.
For those who can afford it, standing wheelchairs are also a great way to avoid or relieve pressure sores. These kind of wheelchairs are quite expensive (several thousands of $), but definitely worth at least renting and trying.