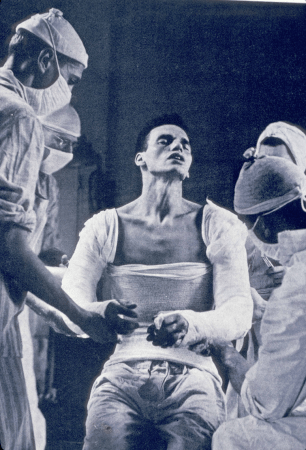
Surgeons and medics apply a plaster-of-paris body cast on an injured soldier. Photo courtesy of the New York Public Library.
During WWII, the incidence of pressure ulcers in young injured soldiers increased as a result of plaster body casts and immobilization splints – an early example of medical device related pressure ulceration. Plaster-of-paris has been used for centuries to treat fractures by immobilizing bones and allowing undisturbed healing. For injuries to the spinal column it was believed that plaster splints prevented hemorrhage and delayed contractures related to paresis.
In WWII plaster was used on a large scale not only to stabilize fractures but also to facilitate safe evacuation of the wounded solider by ambulance or train. Fractures can cause pain and local trauma when evacuation is undertaken over difficult roads as unstable bone fragments scrape against soft tissue. Plaster-of-paris immobilization splints were therefore used in the evacuation hospital close to the site of battle as well as in the general hospital to prepare for the long journey home. The main goal was to relieve pain and prevent further damage to the fracture site, and decrease occurrence of secondary hemorrhage at the site of the fracture. Plaster immobilization was applied in field conditions, often without the benefit of x-rays and by combat medics without training in orthopedics.
Major trauma is often accompanied by blood loss, hypotension and shock, all of which result in decreased tissue perfusion. These physiologic factors, in conjunction with the heavy, rigid plaster splint and unrelieved pressure, frequently led to the tissue ischemia and necrosis. The plaster splint added to vulnerability of skin by causing dryness and inhibiting the removal of sloughed epithelium, leading to dermatitis and infection.
Encasement of the thorax and abdomen limits expansion of the rib cage and eliminates the possibility of therapeutic maneuvers such as chest percussion to assist with clearing secretions. The result was increased risk for pneumonia with decreased oxygen saturation, adding to the risk for pressure ulcers.
As America’s hospitals filled with those injured in the war, caregivers observed a surge in pressure ulcers and their complications resulting directly from the plaster casts. Journals of the day described in detail the devastating sequelae of pressure ulcers including osteomyelitis, pyarthrosis, fever, secondary anemia, and the need for amputation. The postwar period also saw new developments in rehabilitation and therapy. Surgical advances were facilitated by the new miracle drug – penicillin – and included grafts, flap rotation, and excision of boney prominences to prevent recurrence.
This spike in pressure ulcer epidemiology during and post-WWII was an early manifestation of device related pressure ulceration. A medical device related pressure ulcer is defined as a localized injury to the skin or underlying tissue as a result of sustained pressure from a device. This can include tubing, braces, splints, oxygen masks, and prostheses. Prevention of these wounds is often more complicated because the device may be an essential component of treatment. Persons can be more susceptible with impaired sensory perception due to paresis, sedation, neuropathy, or impaired communication.
The problem of device related pressure ulceration is substantial. One article by Apold and Rydrych reported that nearly 1/3 of reported serious pressure ulcers were device related. Prevention measures start with staff education regarding risk, which includes recognition of what a “device” is. Padding under devices should be incorporated whenever feasible. Thorough skin assessment under devices is necessary whenever feasible if not medically contraindicated. As always with pressure ulcer prevention and treatment, family and patient education, communication, and interdisciplinary collaboration is essential.
* * * * * * * * * * * * * *
For more information view my webinar entitled History of Pressure Ulcers & Wound Care: Past, Present, & Future, which is posted on the National Pressure Ulcer Advisory Panel (NPUAP) website and available for ‘on demand’ viewing. View the webinar here.
For NPUAP resources on medical device related pressure ulcers click here.
References for this post included:
Levine JM. Historical prespective: The impact of plaster-of-paris splints on pressure ulcer occurrence in World War II. Advances in Skin & Wound Care 2005; 21 (11): 526-528.
Apold J, Rydrych D. Preventing device-related pressure ulcers: using data to guide statewide change. J Nurs Care Qual 2012; 27(1): 28-34.
For additional material on the history of plaster splinting click here.